The experience gathered so far related to the symptoms of COVID-19 and complications of SARS-CoV-2 infection allows us to conclude that the disease has a different course and that the associated risk to health goes beyond the acute phase of the disease. The health effects of COVID-19 can affect many systems of the body and be distant in time. Convalescents may develop mental and physical complications related to COVID-19. The likely complications following an infection are numerous, which does not mean that every patient will experience them. Let us remember that each of us recovers differently.
The varied course of COVID-19
The course of this virus infection is diverse, and its clinical picture largely depends on patient’s individual characteristics and the dose of the virus. The infection may take the following courses:
- asymptomatic with no changes in well-being,
- mild with fever and upper respiratory symptoms,
- moderate with high fever and lower respiratory symptoms,
- severe with abnormal oxygen saturation, respiratory failure treated in intensive care units,
- critical with multiple organ failure.
Due to the duration of ailments and symptoms, the following can be distinguished:
- acute COVID-19 with symptoms lasting up to 4 weeks,
- long COVID-19 persistent infection with symptoms lasting 4 to 12 weeks,
- post-COVID-19 syndrome with symptoms lasting more than 12 weeks.
SARS-CoV-2 can (but it does not have to) make you seriously ill. For the vast majority of patients the disease is mild, according to the World Health Organization (WHO), as many as 80% of COVID-19 cases are patients, who do not require hospitalization. Deterioration of health depends on the immune response. The proper response of the immune system to SARS-CoV-2 infection enables the fight against the infection, the course of which will correspond to what we defined as mild. An abnormal immune response leads to disease progression to a severe, life-threatening stage, and long-term complications. The course of coronavirus infection is influenced by advanced age, as well as chronic diseases (including obesity), as they are associated with dysfunctions in the functioning of the immune system. Therefore, most fatal victims of the COVID-19 include the elderly, suffering from comorbidities. The body’s excessive response to the virus leads the excessive production of pro-inflammatory cytokines, which promotes disorders of the coagulation system. Increased blood clotting is a particularly dangerous situation for patients with cardiovascular issues. It is worth knowing that the health consequences are associated with an overreaction of the immune system to a viral infection. SARS-CoV-2 infection develops in stages, the danger is that there is an excessive inflammatory reaction in the lungs. The hyperinflammatory reaction in the respiratory system prevents the proper gas exchange. Therefore, a patient in the stage of respiratory failure requires oxygen therapy or connection to a ventilator and mechanical ventilation.
Health consequences
The adverse effects of COVID-19 have been documented for virtually all systems of human body. Pathological lesions occur in:
- cardiovascular system e.g. myocardial infarctions, arrhythmias, heart failures, myocarditis, thromboembolic complications,
- respiratory system e.g. persistent cough, decreased exercise capacity, shortness of breath, pulmonary fibrosis,
- kidneys e.g. acute kidney damage,
- skin e.g. urticarial, vesicular, maculopapular, pseudo-dermal lesions,
- nervous system e.g. loss of sense of smell (anosmia) and taste, headache, muscle pain, stroke, brain fog,
- in the mental sphere e.g. anxiety and depressive disorders, insomnia.
Mental effects
The subject literature indicates a relationship between the excessive production of pro-inflammatory cytokines and the emergence of depression and anxiety in patients who suffered from severe course of COVID-19. It is worth paying attention to another factor that is also not without impact on mental condition. Connecting to a ventilator may be life-saving, but is associated with great anxiety. The patients are unable to breathe, speak, eat or move on their own. We are talking about the time of a pandemic when the patients cannot be accompanied by relatives. The sole companions of such patients are other patients, and the lifesaving devices around them. Involuntary listening to the environment, the sounds of other suffering patients, the alarming sounds of medical equipment typical of intensive care units are a source of anxiety and increase the feeling of stress. Hospitalization alone is an unpleasant experience. It is not surprising that a severely infected patient require emotional and psychological support. They may develop post-traumatic stress disorder (PTSD) associated with their life-threatening condition. Another issue is the emergence or deepening of psychopathological states during the pandemic. Mental balance can be disturbed by illness and the functioning of itself in an extremely stressful and prolonged pandemic situation.

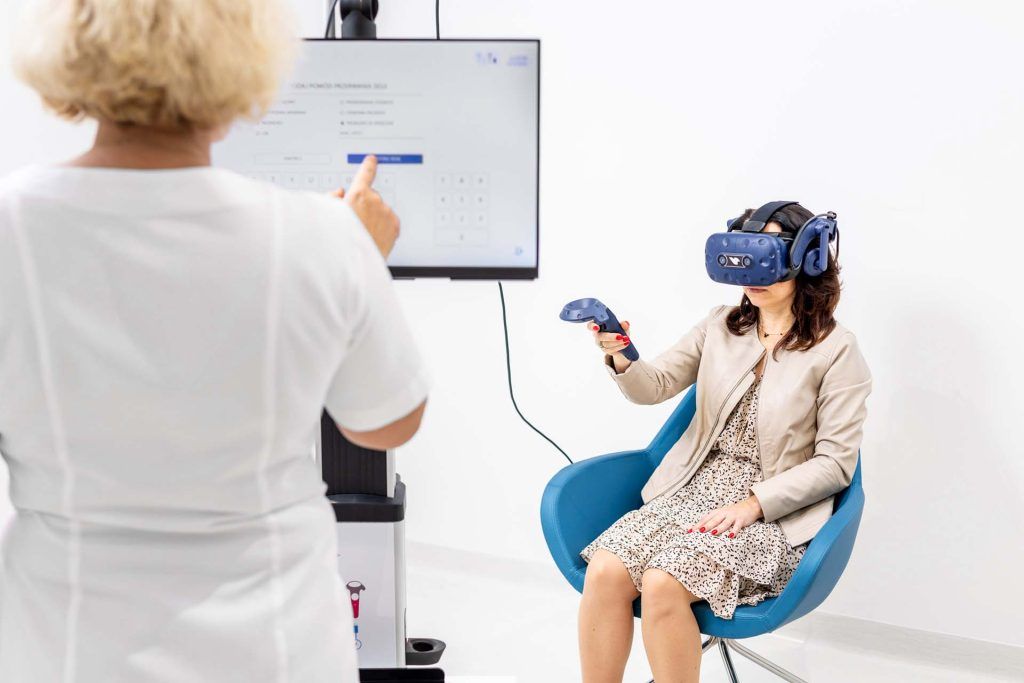
We can restore mental well-being with VR TierOne psychotherapy. This modern method, supporting the treatment of depression, stress and anxiety, will work for people who, due to COVID-19, developed a worse mental functioning.
Neurological complications
Stroke is one possible, dangerous consequence of COVID-19. Stroke is more common in people who suffer from this infection than in the general population. This is because the developing inflammatory reaction promotes deregulation of the coagulation system and the formation of blood clots, and also damage to the endothelium of vessels. As a result of a stroke, brain structures are destroyed, with consequences specific to a stroke, including the risk of post-stroke depression and cognitive decline. A whole of symptoms that has been collectively called brain fog may pose an issue for the convalescents. It may be the result of hypoxia or damage to the brain. Symptoms of brain fog include: disturbance in concentration, memory and orientation, which may persist for up to several months. For convalescents, the feeling of intellectual disability is surprising and disturbing. Inability to perform professional duties negatively affects mental well-being. Reduced cognitive functions, both after stroke, accompanying depression and those called brain fog, can be rehabilitated in a virtual environment, with use of the VR TierOne device.
Comprehensive care
The health effects may persist and lead to limitations in the independent functioning of convalescents. Multi-profile rehabilitation aimed at improving physical and mental health is recommended in case of COVID-19 convalescents. Such comprehensive rehabilitation improves respiratory fitness, exercise and cardiovascular capacity, overall physical fitness, and supports the COVID-19 stricken mental health of patients. Improving well-being is an important objective of post-covid rehabilitation. The sessions in the virtual Garden of Rebirth, allow the patient to experience psychological benefits, and thanks to their relaxing nature, also relaxation on the physiological level. The VR TierOne medical device is perfect for programs intended for convalescents wishing to reduce the health effects of COVID-19.